 
In one patient with severe epistaxis, external carotid artery revascularization led to the healing of the nasal ulcers without need for embolization therapy.įor patients with previous ligations of the external carotid artery and symptomatic AVMs, revascularization of the external carotid artery is an important step in treatment. 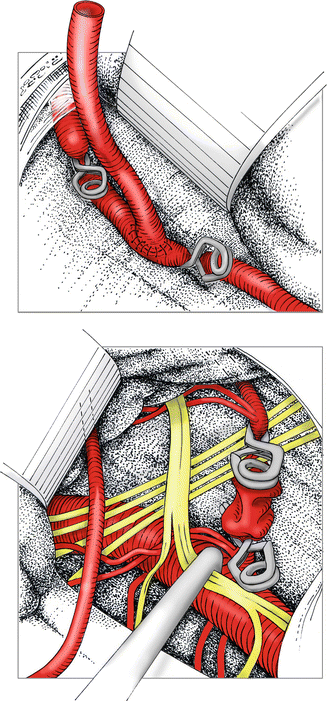
In all, four patients underwent successful embolization therapy. Saphenous vein was used in five reconstructions a polytetrafluoroethylene graft was used in one.Īfter successful arterial reconstruction, massive swelling of the tongue and perioral tissue developed in two patients, which necessitated tracheostomy in one patient and embolization therapy before extubation could be safely performed in the other patient. Six patients with symptoms from cervicofacial arteriovenous malformations required surgical reconstruction of their previously ligated external carotid artery with the anticipation of catheter embolization therapy to the branch vessels feeding the malformation. The purpose of this report is to describe our experience with the treatment of patients with symptomatic unresectable cervicofacial AVMs and previous external carotid artery ligation. Previous ligation of the main feeding vessels prevents catheter access and embolization therapy of the lesion. Percutaneous transcatheter embolization of the nidus of the arteriovenous malformation is now the preferred treatment for symptomatic AVMs that cannot be excised. Rapid enlargement of collateral vessels around the ligature is usually associated with an early return of symptoms. All rights reserved.Until recently, the accepted management of life-threatening complications of unresectable cervicofacial arteriovenous malformations (AVMs) has been ligation of the major feeding vessels, usually the branches or the main trunk of the external carotid artery. Given the dynamic clinical course and potential fatality of PICA dissection, meticulous evaluation, intensive treatment with a diverse range of modalities, and proper follow-up are required for patients with PICA dissection to achieve favorable outcomes.Ĭoil embolization Isolated PICA dissection OA-PICA bypass surgery PICA dissecting aneurysm Trapping.Ĭopyright © 2016 Elsevier Inc. In addition, the other 2 patients (1 in each group) died as a result of major SAH. Although 7 patients showed relatively good outcomes (modified Rankin Scale score, ≤2) after 30 days of follow-up, 1 patient had a final modified Rankin Scale score of 3. Endovascular treatment was performed in 1 patient, who showed rapid progression, aneurysm formation, and conversion to massive SAH within 10 days after the initial attack. Among the 3 patients with infarction, 2 received conservative treatment. Conservative management was performed in the other 2 patients. Dissection was seen at the proximal portion in 8 patients, whereas the remaining 2 patients showed distal PICA dissecting aneurysms.Īmong the 7 patients with hemorrhage, 5 were actively treated (trapping and bypass, 2 patients surgical clipping, 1 patient coil embolization, 2 patients). Ten patients were enrolled, including 7 patients with subarachnoid hemorrhage (SAH) and 3 with PICA territory infarction. We retrospectively reviewed the clinical records of all patients who underwent any PICA dissection treatment in our institute over the last 4 years. However, because of the rarity of these dissections, the optimal treatment has not yet been established. Isolated dissections that develop on the posterior inferior cerebellar artery (PICA) require intensive treatment because of their potential fatality. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
